By Jane Cover, PhD MPH, Research and Evaluation Manager, PATH jcover@path.org
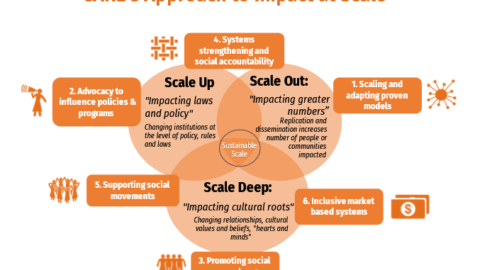
Self-injection of contraception is a new option that enhances women’s autonomy and control over whether and when to have children, while decreasing the time and costs associated with quarterly trips to a clinic. Research on self-injection of the easy-to-use contraceptive subcutaneous DMPA (DMPA-SC, brand name Sayana® Press) from several countries has shown that women are able to self-inject DMPA-SC safely and effectively following training by a health worker. Moving beyond research, there is a clear need to develop approaches to self-injection delivery that can make this new option scalable, sustainable, and accessible to all women.
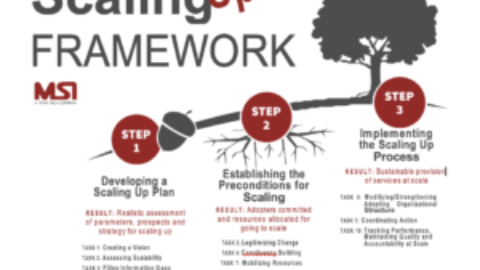
PATH’s Self-Injection Best Practices project is generating evidence and guidance that family planning decision-makers can use to introduce and scale up self-injection in the context of routine programs offer- ing a range of methods. Beginning in 2017, the team applied user-centered design (UCD) approaches to shape self-injection program models being implemented and evaluated across delivery channels in Uganda. Almost 300 health workers were trained to offer self-injection services through: public-sector facilities, community-based delivery, safe spaces for adolescent girls and young women, pharmacies, drug shops, and private clinics. More than 7,000 women became self-injection clients over the first year of implementation, and most took two devices home with them for independent use.
The team designed a monitoring system to capture information on self-injection uptake and the characteristics of women accessing self-injection services. We also conducted an evaluation to identify the most successful program models for DMPA-SC self-injection. Evaluation results will be available later in 2019; in the interim, we have several learnings that can be shared from the experience.
Lessons learned to date:
- A UCD process can save implementers’ time and effort in the long Early UCD collaborations with decision-makers, health workers, and clients helped clarify feasible approaches to self-injection training and follow-up in the context of the Ugandan health system.
- In busy clinic settings, group training may be more feasible than one-on-one training, though guide- lines regarding group size may be needed to ensure quality.
- Women appreciate having a visual job aid they can take home for independent self-injection.
- Incorporating self-injection into HMIS systems is important for quantification, and requires time and provider DMPA-SC doses that are injected at the health facility, those given to women to take home for independent self-injection, and training doses all need to be considered when estimating monthly supplies.
- Especially in the absence of a well-funded and systematic evaluation, supportive supervision is necessary to ensure quality of care, including self-injection training approaches and counseling on a range of options.
The team has also worked to build a collaborative environment for self-injection scale-up in Uganda. PATH coordinates a DMPA-SC scale-up task force and a self-injection advocacy group, both led by the Ministry of Health and composed of several implementing partners. We have also identified national and local self-injection champions who serve as spokespeople for program and policy rollout.
PATH is now developing guidance on how to design scalable self-injection programs, and we plan to disseminate this information globally. The PATH-JSI DMPA-SC Access Collaborative will use these results when supporting countries to develop self-injection approaches appropriate to their budgets and family planning programs. For more information, visit www. path.org/dmpa-sc or email FPoptions@path.org